Introduction
If you recently had a tooth removed and are now feeling strong, throbbing pain that does not seem normal, you may be dealing with a condition called dry socket. Dry socket is a painful problem that can happen after a tooth extraction. It occurs when the protective blood clot that should form in the empty tooth socket either does not develop properly or comes out too soon. When this happens, the bone and nerves underneath are left exposed, leading to intense discomfort.
Many people expect some soreness after a tooth extraction, but dry socket pain is different. It usually feels sharper, deeper, and more severe than normal healing pain. This is why seeing a dentist for dry socket is so important. A dentist can quickly confirm the problem and provide treatment that relieves pain and supports proper healing.
In this guide, you will learn what dry socket is, how it differs from normal healing, the signs that mean you should see a dentist for dry socket, and what treatment involves. You will also discover how to prevent dry socket and what to expect during recovery. The goal is to help you understand the condition clearly and feel confident about seeking care if you need it.
Dry Socket After a Tooth Extraction
Dry socket, also known as alveolar osteitis, is a complication that sometimes occurs after a tooth extraction. When a tooth is removed, the body naturally forms a blood clot in the empty space. This clot plays a vital role in the healing process. It protects the bone and nerves and serves as the foundation for new tissue to grow.
In normal healing, mild swelling and discomfort are expected for a few days. The blood clot stays in place, and the area slowly fills in with new tissue. Pain usually improves each day.
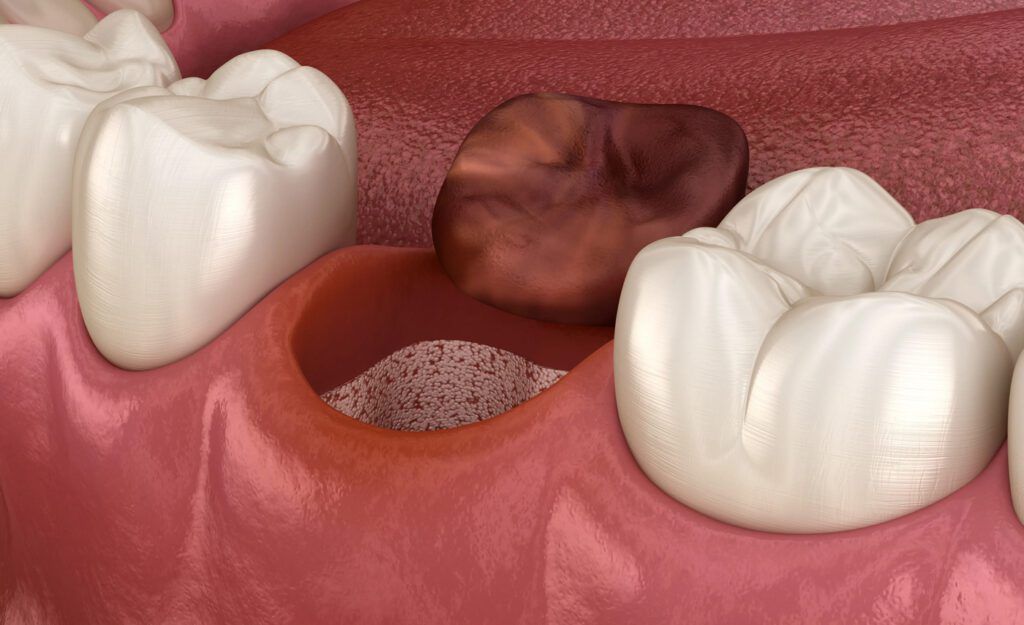
With dry socket, however, the blood clot either fails to form or becomes dislodged too early. This leaves the bone and nerve endings exposed. As a result, the pain can become intense, often starting a few days after the extraction instead of immediately. The pain may spread to the ear, eye, or side of the head on the same side as the extraction.
The blood clot is essential because it acts like a natural bandage. Without it, the healing process slows down and discomfort increases. That is why early care from a dentist for dry socket can make such a big difference. Professional treatment protects the area again and helps restart the healing process in a safe way.
Signs You Should See a Dentist for Dry Socket
Recognizing the symptoms early can help you get treatment before the pain becomes overwhelming. The most common sign is severe pain that begins two to four days after a tooth extraction. While some discomfort is normal, dry socket pain is usually stronger and does not improve with standard pain medicine.
You may also notice that the empty socket looks dry or appears to have a visible bone surface instead of a dark red blood clot. Some people describe it as an empty hole in the gum. This visual change is often a clear signal that the clot has been lost.
Another common symptom is a bad taste in the mouth or an unpleasant smell that does not go away with brushing. This happens because food particles and bacteria can collect in the exposed socket.
The pain from dry socket can radiate beyond the extraction site. It may spread to the jaw, ear, or temple. If the pain feels deep, throbbing, and persistent, it is wise to contact a dentist for dry socket right away.
Urgent dental attention is especially important if the pain is severe, interferes with sleep, or does not improve after a few days. The sooner you receive care, the faster you can find relief.
How a Dentist Diagnoses Dry Socket?
When you visit a dentist for dry socket, the diagnosis process is usually simple and straightforward. The dentist will first ask about your recent tooth extraction, including when it was done and how the healing has felt so far. They may also ask whether you smoke, use straws, or have accidentally disturbed the area.
Next, the dentist will gently examine your mouth. They will look at the extraction site to check whether the blood clot is present. If the socket appears empty or shows exposed bone, this strongly suggests dry socket.
The dentist will also check for signs of infection, such as excessive swelling, pus, or fever. While dry socket itself is not always an infection, it can sometimes lead to one if left untreated. By carefully examining the area, the dentist can rule out other possible complications and confirm the correct diagnosis.
In most cases, no special tests are needed. A visual examination and a discussion of your symptoms are enough for a dentist to determine whether dry socket is the cause of your pain.
What a Dentist Does to Treat Dry Socket?
The main goal of treatment is to relieve pain and protect the exposed area so healing can continue properly. When you see a dentist for dry socket, the first step is usually to clean the empty socket. The dentist will gently rinse it to remove food debris and bacteria. This helps reduce irritation and lowers the risk of infection.
After cleaning the area, the dentist may place a medicated dressing inside the socket. This dressing contains soothing and pain-relieving ingredients. It acts as a protective layer over the exposed bone and nerves. Many patients feel noticeable relief soon after the dressing is placed.
Pain management is another important part of treatment. Your dentist may recommend over-the-counter pain relievers or prescribe medication if the pain is severe. They will also provide instructions on how to care for the area at home.
In some cases, follow-up visits are needed to replace the medicated dressing until the pain subsides and healing progresses well. Each appointment allows the dentist to monitor your recovery and ensure there are no additional problems.
Most people experience significant pain relief within 24 to 48 hours after professional treatment. While full healing may still take some time, seeing a dentist for dry socket greatly improves comfort and speeds up recovery.
Can Dry Socket Heal Without a Dentist?
It is possible for dry socket to heal on its own over time, but the process can be slow and very painful. Without professional care, the exposed bone remains unprotected, and discomfort may continue for days or even weeks.
Delaying treatment increases the risk of complications. Food particles and bacteria can easily enter the empty socket, which may lead to infection. An untreated infection can cause swelling, fever, and more serious health concerns.
Home remedies, such as rinsing with salt water, may provide temporary relief but do not replace the protective function of a blood clot or medicated dressing. Over-the-counter pain medicine might dull the pain slightly, but it does not address the root cause.
In situations where the pain is severe, spreading, or not improving, immediate care from a dentist for dry socket is necessary. Professional treatment not only relieves pain faster but also supports proper healing and reduces the risk of further issues.
How to Prevent Dry Socket After a Tooth Extraction?
Prevention starts with careful aftercare. Following your dentist’s instructions closely after a tooth extraction is the best way to reduce the risk of dry socket. In the first 24 hours, it is important to avoid rinsing vigorously, spitting forcefully, or using straws. These actions can dislodge the blood clot.
Smoking is a major risk factor for dry socket. The suction and chemicals involved in smoking can interfere with clot formation and healing. Avoiding smoking for several days after an extraction significantly lowers your risk.
Good oral hygiene is still important, but it should be done gently. Brush and floss carefully, staying away from the extraction site until your dentist says it is safe. Keeping the rest of your mouth clean helps prevent bacteria from affecting the healing area.
It is also wise to avoid hard, crunchy, or sticky foods in the first few days. Soft foods and plenty of fluids are usually recommended. By protecting the blood clot and keeping the area clean, you can greatly reduce the chance of needing a dentist for dry socket later.
When to Contact a Dentist Immediately?
Some symptoms should not be ignored. If you experience severe or worsening pain a few days after a tooth extraction, it is time to call your dentist. Pain that does not improve with medication or suddenly becomes stronger may indicate dry socket.
Fever or significant swelling in the face or jaw can signal infection. If you notice pus, a persistent bad taste, or difficulty opening your mouth, these are also warning signs.
Understanding the difference between a routine follow-up and an emergency is important. Mild discomfort that improves each day is usually normal. However, intense pain that interferes with eating, speaking, or sleeping deserves prompt attention.
Reaching out to a dentist for dry socket as soon as symptoms appear helps prevent complications and ensures faster relief.
Recovery Timeline After Seeing a Dentist for Dry Socket
After professional treatment, most patients begin to feel better within the first 24 to 48 hours. The medicated dressing placed by the dentist often reduces pain quickly. You may still feel mild soreness, but the sharp, throbbing pain should decrease significantly.
Healing time can vary depending on the individual and the severity of the dry socket. In many cases, the area continues to improve over the next several days. Follow-up visits may be scheduled to check progress and replace dressings if needed.
To support a smoother recovery, follow your dentist’s instructions carefully. Take prescribed medications as directed and avoid activities that could disturb the area. Gentle rinsing, once approved by your dentist, can help keep the socket clean.
Within one to two weeks, most people experience substantial healing. The gum tissue gradually closes over the socket, and discomfort fades. Staying in touch with your dentist during this time ensures that recovery remains on track.
Conclusion
Dry socket is a painful but treatable condition that can develop after a tooth extraction. It happens when the protective blood clot is lost too soon, leaving the bone and nerves exposed. While some discomfort after dental surgery is normal, severe and persistent pain may mean you need to see a dentist for dry socket.
Professional care makes a clear difference. A dentist can clean the area, place a soothing dressing, and guide you through proper healing. Seeking timely treatment reduces pain, prevents complications, and helps you return to normal activities sooner.
If you suspect dry socket, do not wait and hope the pain will disappear on its own. Contacting a dentist for dry socket is the safest and most effective way to protect your oral health and restore comfort. With the right care and attention, healing can move forward smoothly and confidently.
FAQs
How do I know if I need a dentist for dry socket?
If you feel severe, throbbing pain a few days after a tooth extraction and notice an empty-looking socket or bad taste, you likely need professional evaluation.
Can a dentist fix dry socket quickly?
Yes. A dentist for dry socket can provide fast pain relief by cleaning the area and placing a medicated dressing. Many patients feel better within one or two days.
How much does treatment for dry socket cost?
The cost varies by location and clinic, but it is usually affordable. It is best to contact your dental office for exact pricing.
Is dry socket dangerous?
Dry socket is not usually life-threatening, but it is very painful and can lead to infection if untreated. Seeing a dentist prevents complications.
Can I treat dry socket at home?
Home care may ease discomfort slightly, but it cannot replace professional treatment. A dentist for dry socket is the safest option for proper healing.